Head and Neck cancer – 3 – Diagnosis and Staging (1)
HEAD & NECK CANCER PART-3
(All the articles published in past are available at www.shyamhemoncclinic.com/blog/)
Question: Dr. Chiragbhai, thank you for explaining in detail about role of HPV and EBV virus; importance of identifying leukoplakia erythroplakia and early signs/symptoms of these cancers. Can you elaborate more on diagnosis and staging of these cancers?
Ans: Clinical examination remains the most important part of evaluation, including use of mirror or fiberoptic scope, and in some cases examination under anesthesia (later allows better patient relaxation for proper examination). Role of triple endoscopy is not routine. If a patient has neck nodes with unknown primary site, especially when node is in lower part of neck, upper GI endoscopy and bronchoscopy can be added to detect primary.
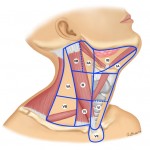
A significant number of patients present with only an enlarged neck node, and biopsy confirms cancer. Location of the node directs clinician to the likely site of primary. This is based on the common drainage patterns. For example, Level I nodes drain oral cavity; Level II drain larynx and nasopharynx ; Level III drain larynx; Level IV and V drain thyroid, nasopharynx, and lesions below clavicle. Neck node involvement is also prognostically significant, reducing cure rate by approximately 50% for given T stage.
Que: What is the role of imaging studies and biopsy?
Ans: Biopsy is done from primary, node or both. A small biopsy from primary if feasible OR fine needle aspiration from node is sufficient in most cases. In case of poorly differentiated tumors or with suspicion of lymphoma, excisional node biopsy may be required. If head and neck primary suspicion is high, a surgeon capable of neck node dissection should be involved in excisional node biopsy.
For imaging, a good quality CT scan with contrast is sufficient in most cases. Some cases may need additional MRI images or only MRI, such as with tongue lesions. MRI is better for soft tissue details and CT is better for bone. Thus both studies are complementary and good radiology centers frequently take few additional images of other modality if required in a given case. For example, when a CT scan is done, they would take few images of MRI to confirm some details, and vice versa.
Incidence of metastatic disease is low for early stage disease, for most sites. Hence a chest x ray is sufficient in most cases for staging. However for advance primary OR with large or bilateral nodes OR in case of Hypopharynx primary, CT scan of chest is required for staging. In case of nasopharynx, there is high incidence of distant metastases, hence CT chest abdomen and Bone scan are required. If a PET-CT is available, it is preferred in such case which includes whole body including bones.
PET-CT is also an important test in case of unknown primary, or when CT scan is showing some inconclusive findings. For most cases, however it is not useful and has false positive and false negative. Also, CT images are not very detailed, hence a good quality CT or MRI is anyway required for neck. Role of PET-CT is however growing for few specific roles. It is highly sensitive and specific for detecting neck nodal metastases, in otherwise normal neck, and is utilized if it will change management, such as radiation planning or neck dissection planning. Also, for initial N2 or N3 node, but now N0 after radiotherapy, PET-CT may help in decision making about node dissection. It should be performed between 8 to 10 weeks after radiotherapy. Newer roles for PET-CT are evolving, such as deciding radiotherapy field.
March 12th 2015.
Dr. Chirag A. Shah; M.D. Oncology/Hematology (USA), 079 26754001. Diplomate American Board of Oncology and Hematology. Ahmedabad. drchiragashah@gmail.com Shyam Hem-Onc Clinic. 402 Galaxy, Near Shivranjani, Opp Jhansi ki Rani BRTS, Ahmedabad. www.shyamhemoncclinic.com
Branden -
This content is excellent but I see that you aren’t using
the full earning potential of your site. You can earn pretty good promoting products related to health and
beauty niche, don’t waste your traffic, just type in google:
Polym’s earning ideas